mitochondria
Basic Researchers Discover Possible Target for Treating Brain Cancer
Posted on by Lawrence Tabak, D.D.S., Ph.D.
Over the years, cancer researchers have uncovered many of the tricks that tumors use to fuel their growth and evade detection by the body’s immune system. More tricks await discovery, and finding them will be key in learning to target the right treatments to the right cancers.
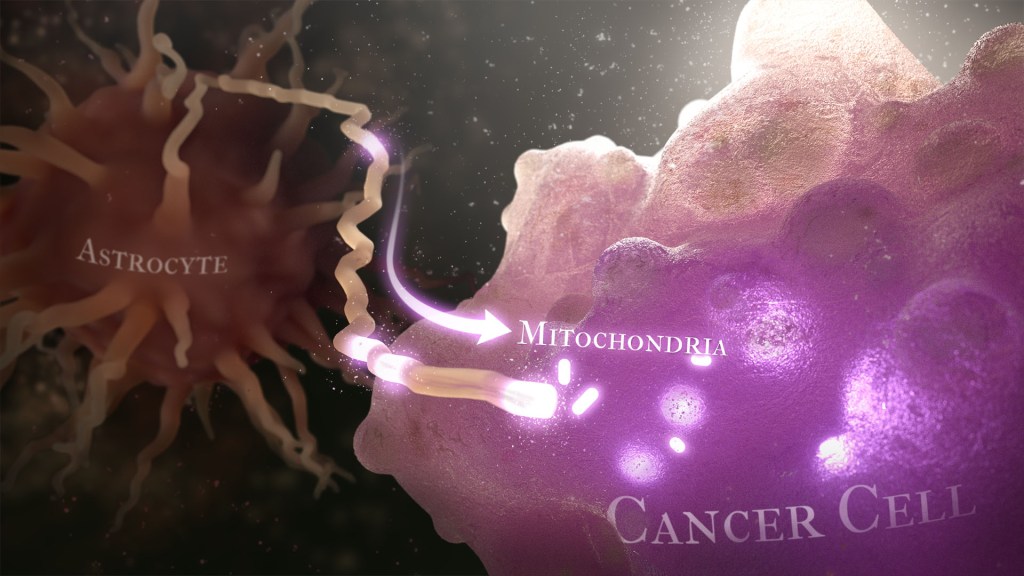
Recently, a team of researchers demonstrated in lab studies a surprising trick pulled off by cells from a common form of brain cancer called glioblastoma. The researchers found that glioblastoma cells steal mitochondria, the power plants of our cells, from other cells in the central nervous system [1].
Why would cancer cells do this? How do they pull it off? The researchers don’t have all the answers yet. But glioblastoma arises from abnormal astrocytes, a particular type of the glial cell, a common cell in the brain and spinal cord. It seems from their initial work that stealing mitochondria from neighboring normal cells help these transformed glioblastoma cells to ramp up their growth. This trick might also help to explain why glioblastoma is one of the most aggressive forms of primary brain cancer, with limited treatment options.
In the new study, published in the journal Nature Cancer, a team co-led by Justin Lathia, Lerner Research Institute, Cleveland Clinic, OH, and Hrvoje Miletic, University of Bergen, Norway, had noticed some earlier studies suggesting that glioblastoma cells might steal mitochondria. They wanted to take a closer look.
This very notion highlights an emerging and much more dynamic view of mitochondria. Scientists used to think that mitochondria—which can number in the thousands within a single cell—generally just stayed put. But recent research has established that mitochondria can move around within a cell. They sometimes also get passed from one cell to another.
It also turns out that the intercellular movement of mitochondria has many implications for health. For instance, the transfer of mitochondria helps to rescue damaged tissues in the central nervous system, heart, and respiratory system. But, in other circumstances, this process may possibly come to the rescue of cancer cells.
While Lathia, Miletic, and team knew that mitochondrial transfer was possible, they didn’t know how relevant or dangerous it might be in brain cancers. To find out, they studied mice implanted with glioblastoma tumors from other mice or people with glioblastoma. This mouse model also had been modified to allow the researchers to trace the movement of mitochondria.
Their studies show that healthy cells often transfer some of their mitochondria to glioblastoma cells. They also determined that those mitochondria often came from healthy astrocytes, a process that had been seen before in the recovery from a stroke.
But the transfer process isn’t easy. It requires that a cell expend a lot of energy to form actin filaments that contract to pull the mitochondria along. They also found that the process depends on growth-associated protein 43 (GAP43), suggesting that future treatments aimed at this protein might help to thwart the process.
Their studies also show that, after acquiring extra mitochondria, glioblastoma cells shift into higher gear. The cancerous cells begin burning more energy as their metabolic pathways show increased activity. These changes allow for more rapid and aggressive growth. Overall, the findings show that this interaction between healthy and cancerous cells may partly explain why glioblastomas are so often hard to beat.
While more study is needed to confirm the role of this process in people with glioblastoma, the findings are an important reminder that treatment advances in oncology may come not only from study of the cancer itself but also by carefully considering the larger context and environments in which tumors grow. The hope is that these intriguing new findings will one day lead to new treatment options for the approximately 13,000 people in the U.S. alone who are diagnosed with glioblastoma each year [2].
References:
[1] GAP43-dependent mitochondria transfer from astrocytes enhances glioblastoma tumorigenicity. Watson DC, Bayik D, Storevik S, Moreino SS, Hjelmeland AB, Hossain JA, Miletic H, Lathia JD et al. Nat Cancer. 2023 May 11. [Published online ahead of print.]
[2] CBTRUS statistical report: Primary brain and other central nervous system tumors diagnosed in the United States in 2011-2015. Ostrom QT, Gittleman H, Truitt G, Boscia A, Kruchko C, Barnholtz-Sloan JS. 2018 Oct 1, Neuro Oncol., p. 20(suppl_4):iv1-iv86.
Links:
Glioblastoma (National Center for Advancing Translational Sciences/NIH)
Brain Tumors (National Cancer Institute/NIH)
Justin Lathia Lab (Cleveland Clinic, OH)
Hrvoje Miletic (University of Bergen, Norway)
NIH Support: National Institute of Neurological Disorders and Stroke; National Center for Advancing Translational Sciences; National Cancer Institute; National Institute of Allergy and Infectious Diseases
The People’s Picks for Best Posts
Posted on by Dr. Francis Collins
It’s 2021—Happy New Year! Time sure flies in the blogosphere. It seems like just yesterday that I started the NIH Director’s Blog to highlight recent advances in biology and medicine, many supported by NIH. Yet it turns out that more than eight years have passed since this blog got rolling and we are fast approaching my 1,000th post!
I’m pleased that millions of you have clicked on these posts to check out some very cool science and learn more about NIH and its mission. Thanks to the wonders of social media software, we’ve been able to tally up those views to determine each year’s most-popular post. So, I thought it would be fun to ring in the New Year by looking back at a few of your favorites, sort of a geeky version of a top 10 countdown or the People’s Choice Awards. It was interesting to see what topics generated the greatest interest. Spoiler alert: diet and exercise seemed to matter a lot! So, without further ado, I present the winners:
2013: Fighting Obesity: New Hopes from Brown Fat. Brown fat, one of several types of fat made by our bodies, was long thought to produce body heat rather than store energy. But Shingo Kajimura and his team at the University of California, San Francisco, showed in a study published in the journal Nature, that brown fat does more than that. They discovered a gene that acts as a molecular switch to produce brown fat, then linked mutations in this gene to obesity in humans.
What was also nice about this blog post is that it appeared just after Kajimura had started his own lab. In fact, this was one of the lab’s first publications. One of my goals when starting the blog was to feature young researchers, and this work certainly deserved the attention it got from blog readers. Since highlighting this work, research on brown fat has continued to progress, with new evidence in humans suggesting that brown fat is an effective target to improve glucose homeostasis.
2014: In Memory of Sam Berns. I wrote this blog post as a tribute to someone who will always be very near and dear to me. Sam Berns was born with Hutchinson-Gilford progeria syndrome, one of the rarest of rare diseases. After receiving the sad news that this brave young man had passed away, I wrote: “Sam may have only lived 17 years, but in his short life he taught the rest of us a lot about how to live.”
Affecting approximately 400 people worldwide, progeria causes premature aging. Without treatment, children with progeria, who have completely normal intellectual development, die of atherosclerotic cardiovascular disease, on average in their early teens.
From interactions with Sam and his parents in the early 2000s, I started to study progeria in my NIH lab, eventually identifying the gene responsible for the disorder. My group and others have learned a lot since then. So, it was heartening last November when the Food and Drug Administration approved the first treatment for progeria. It’s an oral medication called Zokinvy (lonafarnib) that helps prevent the buildup of defective protein that has deadly consequences. In clinical trials, the drug increased the average survival time of those with progeria by more than two years. It’s a good beginning, but we have much more work to do in the memory of Sam and to help others with progeria. Watch for more about new developments in applying gene editing to progeria in the next few days.
2015: Cytotoxic T Cells on Patrol. Readers absolutely loved this post. When the American Society of Cell Biology held its first annual video competition, called CellDance, my blog featured some of the winners. Among them was this captivating video from Alex Ritter, then working with cell biologist Jennifer Lippincott-Schwartz of NIH’s Eunice Kennedy Shriver National Institute of Child Health and Human Development. The video stars a roving, specialized component of our immune system called cytotoxic T cells. Their job is to seek out and destroy any foreign or detrimental cells. Here, these T cells literally convince a problem cell to commit suicide, a process that takes about 10 minutes from detection to death.
These cytotoxic T cells are critical players in cancer immunotherapy, in which a patient’s own immune system is enlisted to control and, in some cases, even cure the cancer. Cancer immunotherapy remains a promising area of research that continues to progress, with a lot of attention now being focused on developing immunotherapies for common, solid tumors like breast cancer. Ritter is currently completing a postdoctoral fellowship in the laboratory of Ira Mellman, Genentech, South San Francisco. His focus has shifted to how cancer cells protect themselves from T cells. And video buffs—get this—Ritter says he’s now created even cooler videos that than the one in this post.
2016: Exercise Releases Brain-Healthy Protein. The research literature is pretty clear: exercise is good for the brain. In this very popular post, researchers led by Hyo Youl Moon and Henriette van Praag of NIH’s National Institute on Aging identified a protein secreted by skeletal muscle cells to help explore the muscle-brain connection. In a study in Cell Metabolism, Moon and his team showed that this protein called cathepsin B makes its way into the brain and after a good workout influences the development of new neural connections. This post is also memorable to me for the photo collage that accompanied the original post. Why? If you look closely at the bottom right, you’ll see me exercising—part of my regular morning routine!
2017: Muscle Enzyme Explains Weight Gain in Middle Age. The struggle to maintain a healthy weight is a lifelong challenge for many of us. While several risk factors for weight gain, such as counting calories, are within our control, there’s a major one that isn’t: age. Jay Chung, a researcher with NIH’s National Heart, Lung, and Blood Institute, and his team discovered that the normal aging process causes levels of an enzyme called DNA-PK to rise in animals as they approach middle age. While the enzyme is known for its role in DNA repair, their studies showed it also slows down metabolism, making it more difficult to burn fat.
Since publishing this paper in Cell Metabolism, Chung has been busy trying to understand how aging increases the activity of DNA-PK and its ability to suppress renewal of the cell’s energy-producing mitochondria. Without renewal of damaged mitochondria, excess oxidants accumulate in cells that then activate DNA-PK, which contributed to the damage in the first place. Chung calls it a “vicious cycle” of aging and one that we’ll be learning more about in the future.
2018: Has an Alternative to Table Sugar Contributed to the C. Diff. Epidemic? This impressive bit of microbial detective work had blog readers clicking and commenting for several weeks. So, it’s no surprise that it was the runaway People’s Choice of 2018.
Clostridium difficile (C. diff) is a common bacterium that lives harmlessly in the gut of most people. But taking antibiotics can upset the normal balance of healthy gut microbes, allowing C. diff. to multiply and produce toxins that cause inflammation and diarrhea.
In the 2000s, C. diff. infections became far more serious and common in American hospitals, and Robert Britton, a researcher at Baylor College of Medicine, Houston, wanted to know why. He and his team discovered that two subtypes of C. diff have adapted to feed on the sugar trehalose, which was approved as a food additive in the United States during the early 2000s. The team’s findings, published in the journal Nature, suggested that hospitals and nursing homes battling C. diff. outbreaks may want to take a closer look at the effect of trehalose in the diet of their patients.
2019: Study Finds No Benefit for Dietary Supplements. This post that was another one that sparked a firestorm of comments from readers. A team of NIH-supported researchers, led by Fang Fang Zhang, Tufts University, Boston, found that people who reported taking dietary supplements had about the same risk of dying as those who got their nutrients through food. What’s more, the mortality benefits associated with adequate intake of vitamin A, vitamin K, magnesium, zinc, and copper were limited to amounts that are available from food consumption. The researchers based their conclusion on an analysis of the well-known National Health and Nutrition Examination Survey (NHANES) between 1999-2000 and 2009-2010 survey data. The team, which reported its data in the Annals of Internal Medicine, also uncovered some evidence suggesting that certain supplements might even be harmful to health when taken in excess.
2020: Genes, Blood Type Tied to Risk of Severe COVID-19. Typically, my blog focuses on research involving many different diseases. That changed in 2020 due to the emergence of a formidable public health challenge: the coronavirus disease 2019 (COVID-19) pandemic. Since last March, the blog has featured 85 posts on COVID-19, covering all aspects of the research response and attracting more visitors than ever. And which post got the most views? It was one that highlighted a study, published last June in the New England Journal of Medicine, that suggested the clues to people’s variable responses to COVID-19 may be found in our genes and our blood types.
The researchers found that gene variants in two regions of the human genome are associated with severe COVID-19 and correspondingly carry a greater risk of COVID-19-related death. The two stretches of DNA implicated as harboring risks for severe COVID-19 are known to carry some intriguing genes, including one that determines blood type and others that play various roles in the immune system.
In fact, the findings suggest that people with blood type A face a 50 percent greater risk of needing oxygen support or a ventilator should they become infected with the novel coronavirus. In contrast, people with blood type O appear to have about a 50 percent reduced risk of severe COVID-19.
That’s it for the blog’s year-by-year Top Hits. But wait! I’d also like to give shout outs to the People’s Choice winners in two other important categories—history and cool science images.
Top History Post: HeLa Cells: A New Chapter in An Enduring Story. Published in August 2013, this post remains one of the blog’s greatest hits with readers. The post highlights science’s use of cancer cells taken in the 1950s from a young Black woman named Henrietta Lacks. These “HeLa” cells had an amazing property not seen before: they could be grown continuously in laboratory conditions. The “new chapter” featured in this post is an agreement with the Lacks family that gives researchers access to the HeLa genome data, while still protecting the family’s privacy and recognizing their enormous contribution to medical research. And the acknowledgments rightfully keep coming from those who know this remarkable story, which has been chronicled in both book and film. Recently, the U.S. Senate and House of Representatives passed the Henrietta Lacks Enhancing Cancer Research Act to honor her extraordinary life and examine access to government-funded cancer clinical trials for traditionally underrepresented groups.
Top Snapshots of Life: A Close-up of COVID-19 in Lung Cells. My blog posts come in several categories. One that you may have noticed is “Snapshots of Life,” which provides a showcase for cool images that appear in scientific journals and often dominate Science as Art contests. My blog has published dozens of these eye-catching images, representing a broad spectrum of the biomedical sciences. But the blog People’s Choice goes to a very recent addition that reveals exactly what happens to cells in the human airway when they are infected with the coronavirus responsible for COVID-19. This vivid image, published in the New England Journal of Medicine, comes from the lab of pediatric pulmonologist Camille Ehre, University of North Carolina at Chapel Hill. This image squeezed in just ahead of another highly popular post from Steve Ramirez, Boston University, in 2019 that showed “What a Memory Looks Like.”
As we look ahead to 2021, I want to thank each of my blog’s readers for your views and comments over the last eight years. I love to hear from you, so keep on clicking! I’m confident that 2021 will generate a lot more amazing and bloggable science, including even more progress toward ending the COVID-19 pandemic that made our past year so very challenging.
NASA Twins Study Reveals Health Effects of Space Flight
Posted on by Dr. Francis Collins
Sending one identical twin into space while the other stays behind on Earth might sound like the plot of a sci-fi thriller. But it’s actually a setup for some truly fascinating scientific research!
As part of NASA’s landmark Twins Study, Scott Kelly became the first U.S. astronaut to spend nearly a year in “weightless” microgravity conditions aboard the International Space Station. Meanwhile, his identical twin, retired astronaut Mark Kelly, remained earthbound. Researchers put both men—who like all identical twins shared the same genetic makeup at birth—through the same battery of biomedical tests to gauge how the human body responds to life in space. The good news for the future of space travel is that the results indicated that health is “mostly sustained” during a prolonged stay in space.
Reporting in the journal Science, the Twins Study team, which included several NIH-funded researchers, detailed many thousands of differences between the Kelly twins at the molecular, cellular, and physiological levels during the 340-day observation period. However, most of Scott’s measures returned to near pre-flight levels within six months of rejoining Mark on Earth.
Over the past nearly 60 years, 559 people have flown in space. While weightless conditions are known to speed various processes associated with aging, few astronauts have remained in space for more than a few months at a time. With up to three year missions to the moon or Mars planned for the future, researchers want to get a better sense of how the human body will hold up under microgravity conditions for longer periods.
To get a more holistic answer, researchers collected a variety of biological samples from the Kelly twins before, during, and after Scott’s spaceflight. All told, more than 300 samples were collected over the course of 27 months.
Multiple labs around the country used state-of-the art tools to examine those samples in essentially every way they could think of doing. Those analyses offer a remarkably detailed view of changes in an astronaut’s biology and health while in space.
With so much data, there were lots of interesting findings to report, including many changes in the expression of Scott’s genes that weren’t observed in his twin. While most of these changes returned to preflight levels within six months of Scott’s return to Earth, about 7 percent of his genes continued to be expressed at different levels. These included some related to DNA repair and the immune system.
Despite those changes in immunity-related gene expression, his immune system appeared to remain fully functional. His body responded to the flu vaccine administered in space just as would be expected back home on Earth.
Scott also had some measurable changes in telomeres—complexes of specialized DNA sequences, RNA, and protein that protect the tips of our chromosomes. These generally shorten a bit each time cells divide. But during the time in space, the telomeres in Scott’s white blood cells measured out at somewhat greater length.
Potentially, this is because some of his stem cells, which are younger and haven’t gone through as many cell divisions, were being released into the blood. Back on Earth, his telomere lengths returned to an average length within six months of his return. Over the course of the study, the earthbound telomeres of his twin brother Mark remained stable.
Researchers also uncovered small but significant changes to Scott’s gut microbiome, the collection of microbes that play important roles in digestion and the immune system. More specifically, there was a shift in the ratio of two major groups of bacteria. Once back on Earth, his microbiome quickly shifted back to its original preflight state.
The data also provided some metabolic evidence suggesting that Scott’s mitochondria, the cellular powerhouses that supply the body with energy, weren’t functioning at full capacity in space. While further study is needed, the NIH-funded team led by Kumar Sharma, University of Texas Health Science Center, San Antonio, suggests that changes in the mitochondria might underlie changes often seen in space to the human cardiovascular system, kidneys, and eyes.
Of course, such a small, two-person study makes it hard to draw any general conclusions about human health in space. But the comparisons certainly help to point us in the right direction. They provide a framework for understanding how the human body responds on a molecular and cellular level to microgravity over time. They also may hold important lessons for understanding human health and precision medicine down here on Earth.
I look forward to future space missions and their contributions to biomedical research. I’m also happy to report, it will be a short wait.
Last year, I highlighted the Tissue Chips in Space Initiative. It’s a unique collaboration between NIH and NASA in which dozens of human tissue chips—tiny, 3D devices bioengineered to model different tissues and organs—will be sent to the International Space Station to study the accelerated aging that occurs in space.
The first tissue chips were sent to the International Space Station last December. And I’m pleased to report that more were aboard recently when the SpaceX Dragon cargo spacecraft made a resupply run to the International Space Station. On May 8, astronauts there successfully completed offloading miniaturized tissue chips of the lungs, bone marrow, and kidneys, enabling more truly unique science in low gravity that couldn’t be performed down here on Earth.
Reference:
[1] The NASA Twins Study: A multidimensional analysis of a year-long human spaceflight. Garrett-Bakelman FE, Darshi M, Green SJ, Gur RC, Lin L, Macias BR, et. al. Science. 2019 Apr 12;364(6436).
Links:
Twins Study (NASA)
Launches and Landings (NASA. Washington, D.C.)
Kumar Sharma (University of Texas Health Science Center, San Antonio)
Tissue Chips in Space (National Center for Advancing Translational Sciences/NIH)
NIH Support: National Institute on Aging; National Institute of Diabetes and Digestive and Kidney Diseases
Snapshots of Life: Mending Broken Hearts
Posted on by Dr. Francis Collins
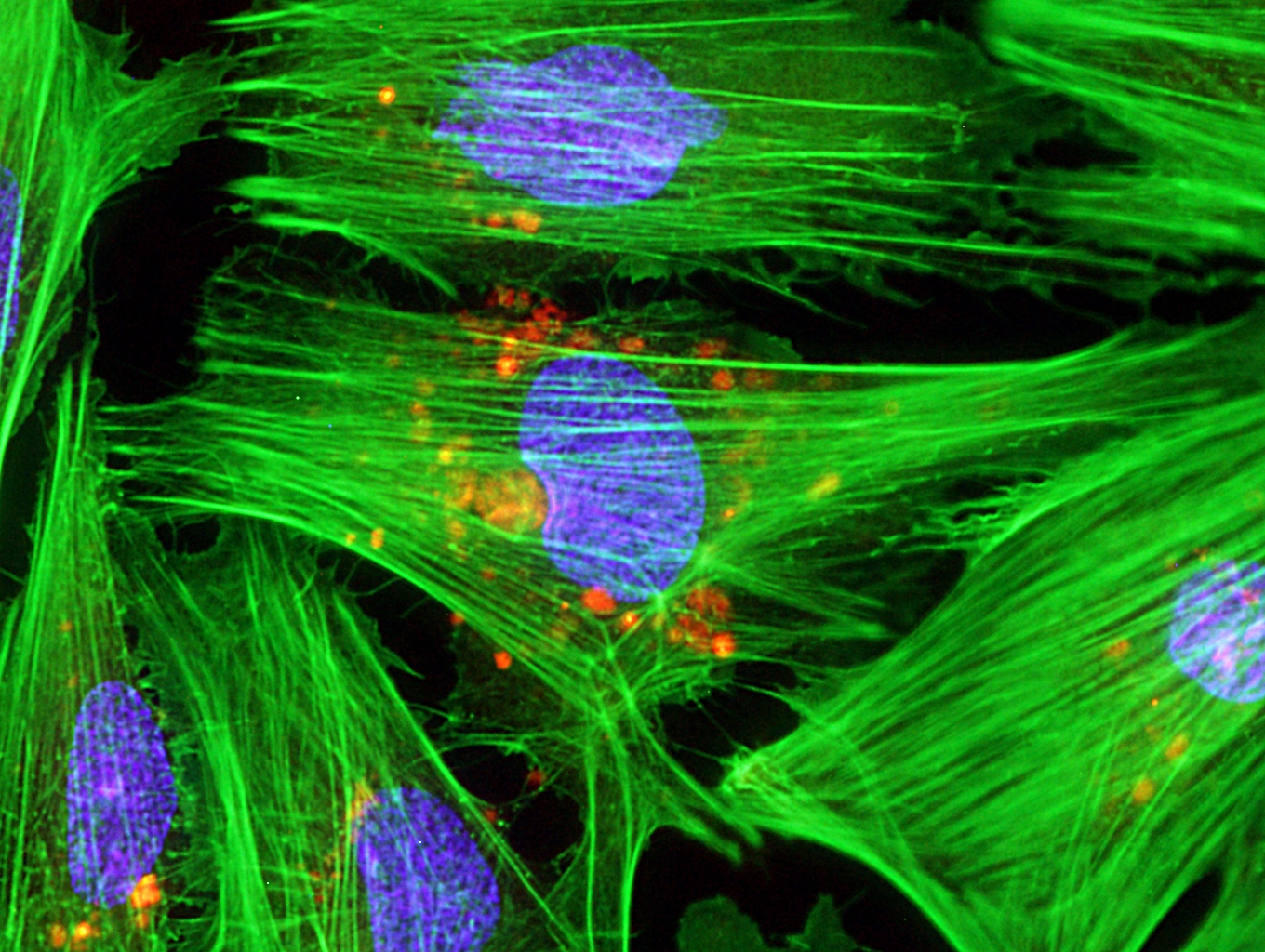
Caption: Micrograph of laboratory-grown rat heart muscle cells. Fluorescent labeling shows mitochondria (red), cytoskeleton (green), and nuclei (blue).
Credit: Credit: Douglas B. Cowan and James D. McCully, Harvard Medical School, Boston
This may not look like your average Valentine’s Day card, but it’s an image sure to warm the hearts of many doctors and patients. Why? This micrograph, a winner in the Federation of American Societies for Experimental Biology’s 2013 BioArt Competition, shows cells that have been specially engineered to repair the damage done by heart attacks—which strike more than 700,000 Americans every year.
Working with rat heart muscle cells grown in a lab dish, NIH-supported bioengineers at Harvard Medical School used transplant techniques to boost the number of tiny powerhouses, called mitochondria, within the cells. If you look closely at the image above, you’ll see the heart muscle cells are tagged in green, their nuclei in blue, and their mitochondria in red.
Brown Fat, White Fat, Good Fat, Bad Fat
Posted on by Dr. Francis Collins

Credit: Patrick Seale, University of Pennsylvania School of Medicine
Fat has been villainized; but all fat was not created equal. Our two main types of fat—brown and white—play different roles. Now, two teams of NIH-funded researchers have enriched our understanding of adipose tissue. The first team discovered the genetic switch that triggers the development of brown fat [1], and the second figured out how the body can recruit white fat and transform it into brown [2].
Why would we want to change white fat into brown? White fat stores energy as large fat droplets, while brown fat has much smaller droplets and is specialized to burn them, yielding heat. Brown fat cells are packed with energy generating powerhouses called mitochondria that contain iron—which gives them their brown color. Infants are born with rich stores of brown fat (about 5% of total body mass) on the upper spine and shoulders to keep them warm. It used to be thought that brown fat disappeared by adulthood—but it turns out we harbor small reserves in our shoulders and neck.
Protein Machines at Work
Posted on by Dr. Francis Collins
This video shows a molecular view of the reactions that take place inside the pyruvate dehydrogenase complex, a protein machine found in the cell’s powerhouse, the mitochondria. 3D imaging of this machine by high-resolution electron microscopy reveals how the different components essential for the reaction are organized. Watch the flexible arms move inside the protein machine as pyruvate (an essential compound made from glucose) gets converted into acetyl-CoA (a precursor to the cell’s energy supply).
Credit: Jacqueline Milne and Sriram Subramaniam, Laboratory of Cell Biology, National Cancer Institute; Donald Bliss, National Library of Medicine; NIH
References:
Molecular architecture and mechanism of an icosahedral pyruvate dehydrogenase complex: a multifunctional catalytic machine. Milne JL, Shi D, Rosenthal PB, Sunshine JS, Domingo GJ, Wu X, Brooks BR, Perham RN, Henderson R, Subramaniam S. EMBO J. 2002 Nov 1;21(21):5587-98.
Molecular structure of a 9-MDa icosahedral pyruvate dehydrogenase subcomplex containing the E2 and E3 enzymes using cryoelectron microscopy. Milne JL, Wu X, Borgnia MJ, Lengyel JS, Brooks BR, Shi D, Perham RN, Subramaniam S. J Biol Chem. 2006 Feb 17;281(7):4364-70.
Extended polypeptide linkers establish the spatial architecture of a pyruvate dehydrogenase multienzyme complex. Lengyel JS, Stott KM, Wu X, Brooks BR, Balbo A, Schuck P, Perham RN, Subramaniam S, Milne JL. Structure. 2008 Jan;16(1):93-103
Science Becomes Art
Posted on by Dr. Francis Collins
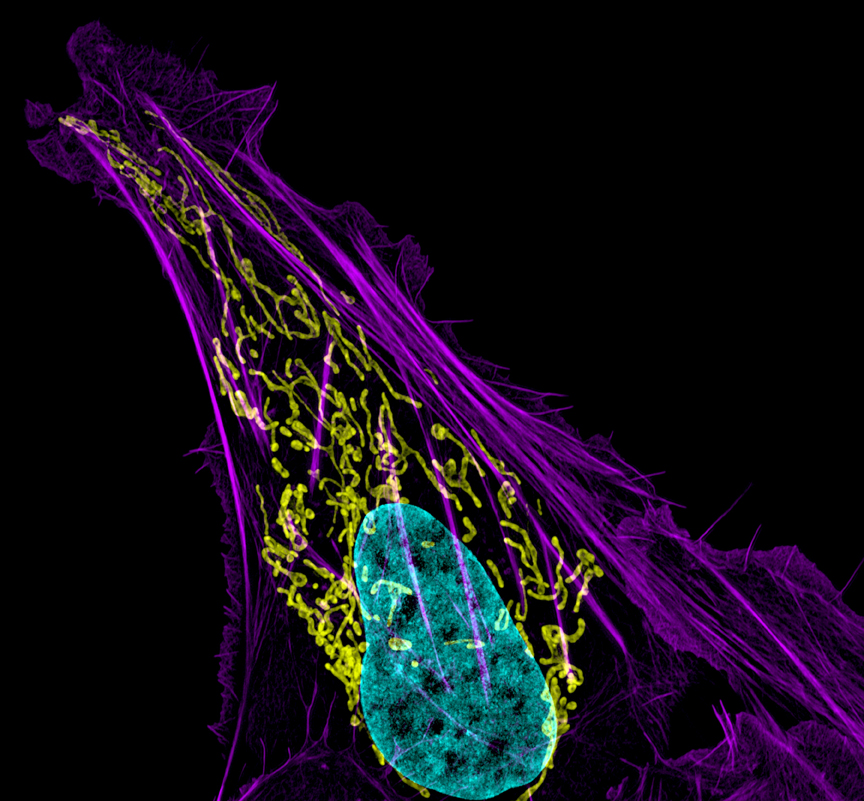
Credit: Dylan T. Burnette, NICHD, NIH
This stunning picture of a human bone cancer cell won artistic accolades: 3rd place in the Nikon Small World Competition. DNA, the blueprint of life, is actually blue in this photo. The yellow squiggles are little powerhouses called mitochondria that generate ATP ‘fuel’ for the cell. The purple wisps are filaments of actin, which help the cell move, keep its shape, and traffic chemicals from one part of the cell to another.
Happy New Year everyone.


