crowdsourcing
Can Smart Phone Apps Help Beat Pandemics?
Posted on by Dr. Francis Collins

In recent weeks, most of us have spent a lot of time learning about coronavirus disease 2019 (COVID-19) and thinking about what’s needed to defeat this and future pandemic threats. When the time comes for people to come out of their home seclusion, how will we avoid a second wave of infections? One thing that’s crucial is developing better ways to trace the recent contacts of individuals who’ve tested positive for the disease-causing agent—in this case, a highly infectious novel coronavirus.
Traditional contact tracing involves a team of public health workers who talk to people via the phone or in face-to-face meetings. This time-consuming, methodical process is usually measured in days, and can even stretch to weeks in complex situations with multiple contacts. But researchers are now proposing to take advantage of digital technology to try to get contact tracing done much faster, perhaps in just a few hours.
Most smart phones are equipped with wireless Bluetooth technology that creates a log of all opt-in mobile apps operating nearby—including opt-in apps on the phones of nearby people. This has prompted a number of research teams to explore the idea of creating an app to notify individuals of exposure risk. Specifically, if a smart phone user tests positive today for COVID-19, everyone on their recent Bluetooth log would be alerted anonymously and advised to shelter at home. In fact, in a recent paper in the journal Science, a British research group has gone so far to suggest that such digital tracing may be valuable in the months ahead to improve our chances of keeping COVID-19 under control [1].
The British team, led by Luca Ferretti, Christophe Fraser, and David Bonsall, Oxford University, started their analyses using previously published data on COVID-19 outbreaks in China, Singapore, and aboard the Diamond Princess cruise ship. With a focus on prevention, the researchers compared the different routes of transmission, including from people with and without symptoms of the infection.
Based on that data, they concluded that traditional contact tracing was too slow to keep pace with the rapidly spreading COVID-19 outbreaks. During the three outbreaks studied, people infected with the novel coronavirus had a median incubation period of about five days before they showed any symptoms of COVID-19. Researchers estimated that anywhere from one-third to one-half of all transmissions came from asymptomatic people during this incubation period. Moreover, assuming that symptoms ultimately arose and an infected person was then tested and received a COVID-19 diagnosis, public health workers would need at least several more days to perform the contact tracing by traditional means. By then, they would have little chance of getting ahead of the outbreak by isolating the infected person’s contacts to slow its rate of transmission.
When they examined the situation in China, the researchers found that available data show a correlation between the roll-out of smart phone contact-tracing apps and the emergence of what appears to be sustained suppression of COVID-19 infection. Their analyses showed that the same held true in South Korea, where data collected through a smart phone app was used to recommend quarantine.
Despite its potential benefits in controlling or even averting pandemics, the British researchers acknowledged that digital tracing poses some major ethical, legal, and social issues. In China, people were required to install the digital tracing app on their phones if they wanted to venture outside their immediate neighborhoods. The app also displayed a color-coded warning system to enforce or relax restrictions on a person’s movements around a city or province. The Chinese app also relayed to a central database the information that it had gathered on phone users’ movements and COVID-19 status, raising serious concerns about data security and privacy of personal information.
In their new paper, the Oxford team, which included a bioethicist, makes the case for increased social dialogue about how best to employ digital tracing in ways the benefit human health. This is a far-reaching discussion with implications far beyond times of pandemic. Although the team analyzed digital tracing data for COVID-19, the algorithms that drive these apps could be adapted to track the spread of other common infectious diseases, such as seasonal influenza.
The study’s authors also raised another vital point. Even the most-sophisticated digital tracing app won’t be of much help if smart phone users don’t download it. Without widespread installation, the apps are unable to gather enough data to enable effective digital tracing. Indeed, the researchers estimate that about 60 percent of new COVID-19 cases in a community would need to be detected–and roughly the same percentage of contacts traced—to squelch the spread of the deadly virus.
Such numbers have app designers working hard to discover the right balance between protecting public health and ensuring personal rights. That includes NIH grantee Trevor Bedford, Fred Hutchinson Cancer Research Center, Seattle. He and his colleagues just launched NextTrace, a project that aims to build an opt-in app community for “digital participatory contact tracing” of COVID-19. Here at NIH, we have a team that is actively exploring the kind of technology that could achieve the benefits without unduly compromising personal privacy.
Bedford emphasizes that he and his colleagues aren’t trying to duplicate efforts already underway. Rather, they want to collaborate with others help to build a scientifically and ethically sound foundation for digital tracing aimed at improving the health of all humankind.
Reference:
[1] Quantifying SARS-CoV-2 transmission suggests epidemic control with digital contact tracing. Ferretti L, Wymant C, Kendall M, Zhao L, Nurtay A, Abeler-Dörner L, Parker M, Bonsall D, Fraser C. Science. 2020 Mar 31. [Epub ahead of print]
Links:
Coronavirus (COVID-19) (NIH)
COVID-19, MERS & SARS (National Institute of Allergy and Infectious Diseases/NIH)
NextTrace (Fred Hutchinson Cancer Research Center, Seattle)
Bedford Lab (Fred Hutchinson Cancer Research Center)
NIH Support: National Institute of General Medical Sciences
Crowdsourcing 600 Years of Human History
Posted on by Dr. Francis Collins
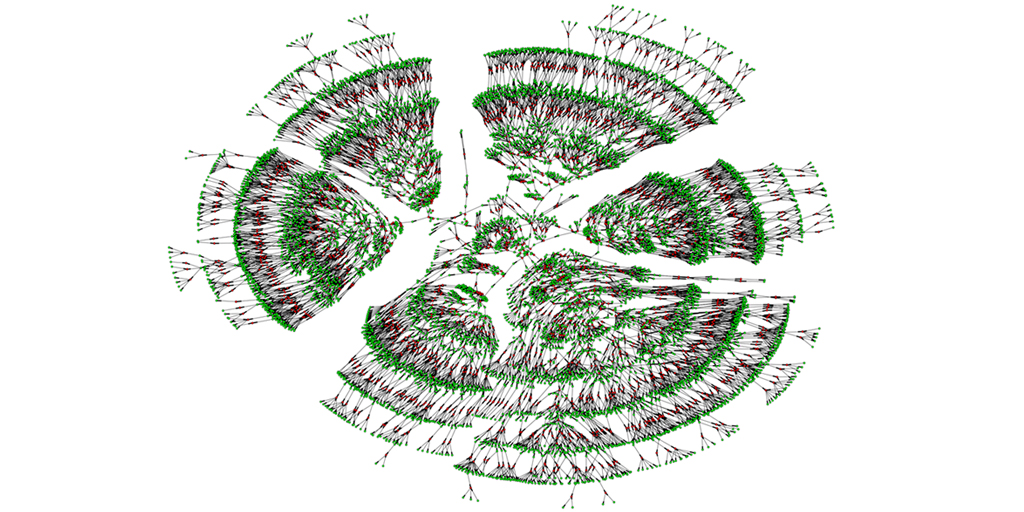
Caption: A 6,000-person family tree, showing individuals spanning seven generations (green) and their marital links (red).
Credit: Columbia University, New York City
You may have worked on constructing your family tree, perhaps listing your ancestry back to your great-grandparents. Or with so many public records now available online, you may have even uncovered enough information to discover some unexpected long-lost relatives. Or maybe you’ve even submitted a DNA sample to one of the commercial sources to see what you could learn about your ancestry. But just how big can a family tree grow using today’s genealogical tools?
A recent paper offers a truly eye-opening answer. With permission to download the publicly available, online profiles of 86 million genealogy hobbyists, most of European descent, the researchers assembled more than 5 million family trees. The largest totaled more than 13 million people! By merging each tree from the crowd-sourced and public data, including the relatively modest 6,000-person seedling shown above, the researchers were able to go back 11 generations on average to the 15th century and the days of Christopher Columbus. Doubly exciting, these large datasets offer a powerful new resource to study human health, having already provided some novel insights into our family structures, genes, and longevity.
Got a Great Research Idea? “All of Us” Wants to Hear It!
Posted on by Dr. Francis Collins
 One of the boldest undertakings that NIH has ever attempted, the All of Us Research Program has been hard at work in a “beta” testing phase, and is now busy gearing up for full recruitment in the spring. This historic effort will enroll 1 million or more people in the United States to share information about their health, habits, and what it’s like where they live. This information will be part of a resource that scientists can use to accelerate research and improve health. How? By taking into account individual differences in lifestyle, environment, and biology, researchers will uncover paths toward realizing the full potential of precision medicine.
One of the boldest undertakings that NIH has ever attempted, the All of Us Research Program has been hard at work in a “beta” testing phase, and is now busy gearing up for full recruitment in the spring. This historic effort will enroll 1 million or more people in the United States to share information about their health, habits, and what it’s like where they live. This information will be part of a resource that scientists can use to accelerate research and improve health. How? By taking into account individual differences in lifestyle, environment, and biology, researchers will uncover paths toward realizing the full potential of precision medicine.
Before embarking on this adventure, All of Us is reaching out to prospective researchers, community organizations, and citizen scientists—including people just like you—to get their input. Imagine that the project has already enrolled 1 million participants from all over the country and from diverse backgrounds. Imagine that they have all agreed to make available their electronic health records, to put on wearable sensors that can track body physiology and environmental exposures, and to provide blood samples for lab testing, including DNA analysis. Is there a particular research question that you think All of Us could help answer? Possible topics include risks of disease, factors that promote wellness, and research on human behavior, prevention, exercise, genetics, environmental health effects, health disparities, and more. To submit an idea, just go to this special All of Us web page.
Snapshots of Life: A Colorful Look Inside the Retina
Posted on by Dr. Francis Collins

Credit: Amy Robinson, Alex Norton, William Silversmith, Jinseop Kim, Kisuk Lee, Aleks Zlasteski, Matt Green, Matthew Balkam, Rachel Prentki, Marissa Sorek, Celia David, Devon Jones, and Doug Bland, Massachusetts Institute of Technology, Cambridge, MA; Sebastian Seung, Princeton University, Princeton, NJ
This eerie scene might bring back memories of the computer-generated alien war machines from Steven Spielberg’s War of the Worlds thriller. But what you’re seeing is a computer-generated depiction of a quite different world—the world inside the retina, the light-sensitive tissue that lines the back of the eye. The stilt-legged “creatures” are actually ganglion nerve cells, and what appears to be their long “noses” are fibers that will eventually converge to form the optic nerve that relays visual signals to the brain. The dense, multi-colored mat near the bottom of the image is a region where the ganglia and other types of retinal cells interact to convey visual information.
What I find particularly interesting about this image is that it was produced through the joint efforts of people who played EyeWire, an internet crowdsourcing game developed in the lab of computational neuroscientist Sebastian Seung, now at Princeton University in New Jersey. Seung and his colleagues created EyeWire using a series of high-resolution microscopic images of the mouse retina, which were digitized into 3D cubes containing dense skeins of branching nerve fibers. It’s at this point where the crowdsourcing came in. Online gamers—most of whom aren’t scientists— volunteered for a challenge that involved mapping the 3D structure of individual nerve cells within these 3D cubes. Players literally colored-in the interiors of the cells and progressively traced their long extensions across the image to distinguish them from their neighbors. Sounds easy, but the branches are exceedingly thin and difficult to follow.
Epilepsy Research Benefits from the Crowd
Posted on by Dr. Francis Collins
 For millions of people with epilepsy, life comes with too many restrictions. If they just had a reliable way to predict when their next seizure will come, they could have a chance at leading more independent and productive lives.
For millions of people with epilepsy, life comes with too many restrictions. If they just had a reliable way to predict when their next seizure will come, they could have a chance at leading more independent and productive lives.
That’s why it is so encouraging to hear that researchers have developed a new algorithm that can predict the onset of a seizure correctly 82 percent of the time. Until recently, the best algorithm was hardly better than flipping a coin, leading some to speculate that seizures are random neurological events that can’t be predicted at all. But the latest leap forward shows that seizures certainly can be predicted, and our research efforts are headed in the right direction to make them even more predictable. The other big news is how this new algorithm was developed: it’s the product of a crowdsourcing competition.
Crowdsourcing Therapeutic Molecules for Drug Discovery
Posted on by Dr. Francis Collins

Caption: The Discovering New Therapeutic Uses for Existing Molecules pilot program matches researchers with pharmaceutical compounds to explore new treatments for patients
Developing a drug takes time and money: on the average, around 14 years and $2 billion or more. More than 95 percent of the drugs fail during development. Even those that go all the way to large and expensive clinical trials in humans frequently don’t make the cut—perhaps because they weren’t quite as effective as they were supposed to be, had undesirable side effects, or didn’t align with the developer’s business priorities. But some of these compounds may have surprising therapeutic properties that have not yet been fully exploited. It would be a wasted opportunity not to take another look at them and test them for effectiveness in other conditions.
For that reason, our National Center for Advancing Translational Sciences (NCATS), with financial support from the NIH Common Fund, launched a pilot program to discover new therapeutic uses for existing molecules. Today we are awarding $12.7 million to nine academic institutions to reexamine a collection of compounds developed by major pharmaceutical companies and test them as treatments for diseases, both common and rare: from alcoholism and Alzheimer’s disease to Duchenne muscular dystrophy and schizophrenia.
